Welcome message
It is our great pleasure to welcome you to the 18th Global Conference on Nephrology and Infectious Diseases, taking place on August 25–26, 2026, in Amsterdam, Netherlands.
This conference brings together leading nephrologists, infectious disease specialists, researchers, clinicians, and healthcare professionals from around the world to share knowledge and discuss the latest scientific developments at the intersection of kidney health and infectious diseases. Centered around the theme “Renal Complications of Viral, Bacterial, Fungal, and Parasitic Infections,” the conference aims to highlight emerging challenges, innovative diagnostic strategies, and advanced treatment approaches that address infection-related kidney disorders.
Through keynote lectures, scientific sessions, and interactive discussions, participants will explore a wide range of topics including emerging infectious diseases, renal pathology, novel therapeutic approaches, and advancements in clinical management. This platform is designed to encourage collaboration, inspire new research ideas, and strengthen global partnerships that advance patient care.
Set in the dynamic and innovative city of Amsterdam, this conference offers not only an enriching scientific experience but also an opportunity to connect with peers, exchange ideas, and build meaningful professional relationships in an inspiring international setting.
We are honored to have you join us and look forward to your active participation in making the 18th Global Conference on Nephrology and Infectious Diseases a successful and impactful event.
About conference
The 18th Global Conference on Nephrology and Infectious Diseases 2026 will be held on August 25–26, 2026, in Amsterdam, Netherlands.
This conference will bring together leading experts, researchers, clinicians, and healthcare professionals from around the world who are dedicated to advancing knowledge in the fields of nephrology and infectious diseases. It will serve as a platform for scientific exchange, collaboration, and discussion on current challenges and emerging developments in kidney health and infection-related complications.
Centered around the theme “Renal Complications of Viral, Bacterial, Fungal, and Parasitic Infections,” the conference will explore the complex interactions between infectious diseases and kidney function. The program will cover a diverse range of topics, including the latest advancements in treatment modalities, emerging infectious diseases, renal pathology, and innovative diagnostic and therapeutic approaches.
This event provides an excellent opportunity for clinicians, researchers, academics, and industry professionals to engage with cutting-edge research, exchange ideas with global experts, and establish collaborations that will contribute to improving patient care and advancing medical science.
Hosted in the vibrant city of Amsterdam, the conference also offers an inspiring environment to connect with peers while exploring new perspectives and innovations in nephrology and infectious diseases.
Why Attend GLOBAL INFECTIONS 2026
-
Latest updates on nephrology and infection-related kidney diseases
-
Insights into renal complications caused by viral, bacterial, fungal, and parasitic infections
-
Advances in diagnostics, treatment strategies, and preventive approaches in kidney infections
-
Expert talks from leading nephrologists and infectious disease specialists
-
Networking opportunities with global healthcare professionals and researchers
-
Case-based discussions on infection-related renal disorders and clinical management
-
Opportunities for career, research, and academic growth
-
Platform to exchange ideas and build international collaborations.
Target Audience
-
Nephrologists
-
Infectious Disease Specialists
-
Urologists
-
Internal Medicine Physicians
-
Renal Transplant Surgeons
-
Dialysis Technicians and Dialysis Nurses
-
Critical Care and ICU Specialists
-
Clinical Researchers and Scientists
-
Pharmacists and Clinical Pharmacologists
-
Medical Coders and Healthcare Administrators
-
Medical Students, Residents, and Fellows
-
Biomedical Engineers (Renal Devices & Dialysis Equipment)
-
Public Health Professionals
-
Healthcare Policy Makers
-
Industry Professionals (Medical Devices & Pharmaceuticals)
Sessions
-
Advances in Chronic Kidney Disease (CKD) Management: Advances in Chronic Kidney Disease (CKD) management focus on early detection and personalized treatment. Innovations in biomarkers and imaging techniques allow for earlier diagnosis, improving patient outcomes. Novel therapeutic approaches, including SGLT2 inhibitors and non-steroidal mineralocorticoid receptor antagonists, have shown efficacy in slowing CKD progression. Additionally, personalized medicine, leveraging genetic and molecular insights, enables tailored treatment plans. Integration of artificial intelligence and machine learning enhances predictive analytics, optimizing patient care. Comprehensive management strategies addressing comorbid conditions, lifestyle modifications, and patient education are crucial, aiming to reduce CKD burden and improve quality of life for affected individuals.
-
Renal Replacement Therapy: Innovations and Challenges: Renal replacement therapy (RRT) has seen significant innovations, including advancements in dialysis technology and kidney transplantation. Improved hemodialysis and peritoneal dialysis techniques enhance patient outcomes and quality of life. Wearable and portable dialysis devices offer greater mobility and convenience. In transplantation, advances in immunosuppressive therapies reduce rejection rates and improve graft longevity. Challenges remain, such as organ shortages, complications from long-term dialysis, and disparities in access to RRT. Ongoing research focuses on bioengineered kidneys and xenotransplantation as potential future solutions. Addressing these challenges requires a multidisciplinary approach to enhance patient care and expand access to life-saving treatments.
-
Artificial Intelligence and Machine Learning in Nephrology: Artificial intelligence (AI) and machine learning (ML) are revolutionizing nephrology by enhancing diagnostics, treatment, and patient management. AI algorithms analyze large datasets to predict kidney disease progression, enabling early intervention. Machine learning models improve the accuracy of renal imaging and pathology, facilitating precise diagnosis. Personalized treatment plans are developed using AI-driven insights from patient data, optimizing therapy outcomes. AI also aids in managing dialysis by predicting complications and optimizing scheduling. Despite these advancements, challenges like data privacy, algorithm bias, and the need for large, high-quality datasets remain. Continuous research and collaboration are essential to fully realize AI's potential in nephrology.
-
Genetic and Molecular Insights in Nephrology: Genetic and molecular insights are transforming nephrology by uncovering the underlying mechanisms of kidney diseases. Advances in genomics and precision medicine allow for the identification of genetic mutations linked to conditions such as polycystic kidney disease and focal segmental glomerulosclerosis. Molecular profiling aids in diagnosing and classifying kidney disorders, leading to more targeted treatments. Pharmacogenomics tailors therapies based on individual genetic profiles, enhancing efficacy and reducing adverse effects. Research into epigenetic modifications and gene therapies holds promise for novel interventions. These insights drive a shift towards personalized nephrology, improving patient outcomes through tailored prevention and treatment strategies.
-
Cardio-Renal Syndromes: Cardio-renal syndromes (CRS) represent a complex interplay between heart and kidney diseases, where dysfunction in one organ adversely affects the other. CRS is categorized into five types, encompassing acute and chronic conditions in both organs. Understanding the bidirectional nature of CRS is crucial for effective management. Innovations in diagnostics, such as biomarkers and imaging techniques, enable early detection and better risk stratification. Treatment strategies focus on integrated care, involving fluid management, blood pressure control, and addressing underlying causes like diabetes and hypertension. Multidisciplinary approaches and personalized medicine are key to improving outcomes for patients with cardio-renal syndromes.
-
Viral & Bacterial Infectious Disease: Viral and bacterial infectious diseases are major global health concerns, differing in their biological characteristics and treatment approaches. Viruses, such as influenza, HIV, and COVID-19, invade host cells to replicate, often leading to acute or chronic illnesses. Bacterial infections, like tuberculosis, streptococcus, and salmonella, involve single-celled organisms that can proliferate in various body tissues, causing localized or systemic diseases. Treatment strategies vary: antiviral medications target viral replication mechanisms, while antibiotics inhibit bacterial growth or kill bacteria outright. Addressing these diseases requires robust vaccination programs, antimicrobial stewardship, and public health measures to prevent transmission and manage outbreaks effectively.
-
Fungal & Parasitic Infectious Disease: Fungal and parasitic infectious diseases pose significant health challenges globally, impacting millions each year. Fungal infections, such as candidiasis, aspergillosis, and cryptococcosis, thrive in specific environmental conditions and can affect various organs, particularly in immunocompromised individuals. Parasitic diseases, like malaria, leishmaniasis, and schistosomiasis, are caused by protozoa or worms and often spread through vectors or contaminated water. Diagnosis relies on microscopy, serology, and molecular tests, while treatment involves antifungal medications for fungi and antiparasitic drugs for parasites. Prevention strategies include vector control, hygiene measures, and targeted treatments in endemic regions, aiming to reduce morbidity and mortality associated with these diseases.
-
Emerging & Infectious Disease: Emerging infectious diseases (EIDs) are newly identified or re-emerging pathogens that pose significant public health threats due to their unpredictable nature and potential for rapid spread. Examples include Ebola virus, Zika virus, and novel influenza strains like H1N1 and avian flu. Factors contributing to their emergence include ecological changes, urbanization, global travel, and microbial evolution. Detecting and responding to EIDs require robust surveillance systems, rapid diagnostic tools, and coordinated international efforts. Effective management involves containment measures, development of vaccines and therapeutics, and public awareness campaigns to mitigate transmission risks and prevent pandemics, highlighting the importance of preparedness and response strategies.
-
Pediatric Infectious Disease: Pediatric infectious diseases encompass a wide range of conditions affecting children, from common illnesses like respiratory tract infections and gastroenteritis to more serious diseases such as meningitis, measles, and pneumonia. Children, especially infants and young toddlers, are particularly vulnerable due to developing immune systems and close contact in daycare or school settings. Diagnosis involves clinical evaluation, laboratory tests, and sometimes imaging studies. Treatment often includes antibiotics for bacterial infections and supportive care for viral illnesses. Vaccination plays a crucial role in preventing many pediatric infections. Addressing pediatric infectious diseases requires pediatric-specific healthcare approaches, including age-appropriate treatments and vaccination schedules.
-
Veterinary Infectious Disease: Veterinary infectious diseases affect animals, impacting animal health, welfare, and agricultural economies. These diseases can also pose risks to human health through zoonotic transmission. Examples include rabies, foot-and-mouth disease, and avian influenza. Diagnosis involves veterinary clinical examination, laboratory testing, and surveillance programs. Management strategies include vaccination, quarantine measures, and treatment with antimicrobials or antiparasitics. Prevention focuses on biosecurity measures, animal husbandry practices, and public health education. Veterinary infectious disease research aims to understand disease dynamics, improve diagnostic tools, and develop effective vaccines and therapies. Collaboration between veterinary and human health sectors is essential for holistic disease control and prevention efforts.
-
Molecular Bacteriology Infection: Molecular bacteriology plays a critical role in understanding bacterial infections at the molecular level, advancing diagnostics, treatment, and prevention strategies. It involves studying bacterial genetics, virulence factors, antibiotic resistance mechanisms, and host-pathogen interactions. Techniques such as polymerase chain reaction (PCR), whole genome sequencing (WGS), and bioinformatics analysis are used to identify bacterial species, characterize their genetic diversity, and track transmission pathways. This knowledge informs the development of new diagnostic tests, targeted therapies, and vaccines. Molecular bacteriology also enhances surveillance efforts, guiding public health interventions to control outbreaks and combat antimicrobial resistance, ensuring effective management of bacterial infections.
-
Vaccination for Infectious Diseases: Vaccination is a crucial public health strategy to prevent infectious diseases by stimulating the immune system to develop protective immunity against specific pathogens. Vaccines contain weakened or killed forms of the microorganism or their proteins, which safely mimic infection without causing illness. This primes the immune system to recognize and respond rapidly if exposed to the actual pathogen, preventing infection or reducing its severity. Vaccination programs target a range of diseases such as measles, polio, influenza, and COVID-19, promoting herd immunity and reducing transmission within communities. Continuous research and monitoring ensure vaccines are safe, effective, and accessible worldwide, saving millions of lives annually.
-
Diagnosis, Management and Treatment of Infections: Diagnosis, management, and treatment of infections are multifaceted processes crucial for effective patient care. Diagnosis involves clinical assessment, laboratory tests (such as microbiological cultures and molecular diagnostics), and imaging studies to identify the causative agent and determine the extent of infection. Management includes supportive care, antimicrobial therapy tailored to the specific pathogen and patient characteristics, and infection control measures to prevent spread. Treatment strategies aim to alleviate symptoms, eradicate the infection, and prevent complications, while minimizing antibiotic resistance and adverse effects. Multidisciplinary collaboration among healthcare providers ensures comprehensive care, optimizing outcomes for patients with infectious diseases.
-
Infection Control in Nephrology Units: Infection control in nephrology units is critical due to the heightened susceptibility of patients undergoing dialysis and kidney transplantation. Key measures include strict adherence to hand hygiene protocols, sterile technique during procedures, and regular environmental cleaning and disinfection. Screening for infections at admission and during treatment helps detect asymptomatic carriers. Isolation precautions are implemented for patients with multidrug-resistant organisms or transmissible infections. Staff education on infection prevention practices and surveillance programs for monitoring infection rates are essential. Collaborative efforts between nephrologists, infectious disease specialists, and infection control teams ensure comprehensive strategies to minimize healthcare associated infections and promote patient safety in nephrology settings.
-
Impact of COVID-19 on Kidney Health: The COVID-19 pandemic has had a profound impact on kidney health, with the virus causing direct kidney injury and exacerbating pre-existing kidney conditions. COVID-19 patients commonly experience acute kidney injury (AKI), often requiring dialysis, due to virus-induced inflammation and clotting disorders affecting renal function. Long-term effects include persistent kidney damage and increased risk of chronic kidney disease (CKD) progression in recovered patients. COVID-19 vaccination campaigns aim to reduce severe cases and associated kidney complications. Ongoing research focuses on understanding the virus's renal effects, improving treatment strategies for kidney-related COVID-19 complications, and addressing long-term kidney health outcomes in survivors.
-
Telemedicine in Nephrology and Infectious Diseases: Telemedicine has revolutionized nephrology and infectious disease care by enabling remote patient monitoring, consultations, and follow-ups. In nephrology, telemedicine facilitates regular assessment of dialysis patients' vital signs, medication management, and dietary counseling, reducing the need for in-person visits and improving access to care, especially in rural or underserved areas. For infectious diseases, telemedicine supports timely diagnosis through virtual consultations, allowing early intervention and reducing transmission risks in outpatient settings. Challenges include ensuring patient privacy, technology accessibility, and regulatory compliance. Continued integration of telemedicine into practice enhances healthcare delivery, patient outcomes, and healthcare system efficiency in nephrology and infectious diseases.
-
Health Disparities in Nephrology and Infectious Diseases: Health disparities in nephrology and infectious diseases highlight inequalities in healthcare access, outcomes, and treatment among diverse populations. Factors such as socioeconomic status, race, ethnicity, and geographic location contribute to disparities in disease prevalence, progression, and mortality rates. In nephrology, disparities manifest in delayed diagnosis, limited access to transplantation, and poorer outcomes for minority and low-income patients. Similarly, in infectious diseases, disparities impact vaccination rates, access to diagnostic tools, and treatment options. Addressing health disparities requires targeted interventions, culturally sensitive care approaches, and policy reforms to ensure equitable access to quality healthcare and improve health outcomes across all communities.
Market Analysis
The global nephrology and infectious diseases market is expected to grow steadily over the next several years, driven by the increasing burden of infection-related kidney complications and the rising prevalence of kidney diseases worldwide. The market is projected to reach approximately $175 billion by 2030, increasing from nearly $130 billion in 2026, at a compound annual growth rate (CAGR) of around 7.5%. This growth is largely fueled by the growing incidence of viral, bacterial, fungal, and parasitic infections that can lead to acute kidney injury (AKI) and chronic kidney disease (CKD), along with improvements in healthcare infrastructure and expanding access to advanced diagnostic technologies.
Infection-associated renal disorders are becoming an increasingly important focus within nephrology research and clinical practice. Conditions such as infection-induced AKI, sepsis-related kidney injury, and renal complications linked to viral infections are gaining greater attention. This segment alone is expected to grow from approximately $45 billion in 2026 to nearly $65 billion by 2031, supported by advances in antimicrobial therapies, improved critical care management, and the integration of infection control strategies into nephrology care. At the same time, the nephrology therapeutics and anti-infective drug market is projected to expand significantly, while renal diagnostics and biomarker technologies are anticipated to grow at a faster pace due to the increasing demand for early detection and AI-supported diagnostic tools.
Regionally, North America continues to lead the market due to its advanced healthcare systems, strong research infrastructure, and early adoption of innovative therapies. Meanwhile, the Asia–Pacific region is expected to experience the fastest growth, driven by rising healthcare awareness, a higher prevalence of infectious diseases, and improving access to kidney care services. Overall, the nephrology and infectious diseases sector is positioned for substantial growth, supported by technological advancements, rising disease prevalence, and increasing investments in research and healthcare infrastructure aimed at improving patient outcomes worldwide.
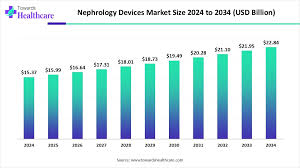
The global nephrology devices market is expected to grow steadily over the next decade, increasing from $15.37 billion in 2024 to approximately $22.84 billion by 2034, reflecting the rising demand for advanced dialysis systems, renal monitoring technologies, and early diagnostic tools. This growth is driven by the increasing prevalence of kidney diseases, infection-related renal complications, and technological advancements in renal care devices.
Major Global Infectious Disease Societies
-
Infectious Diseases Society of America (IDSA)
-
International Society for Infectious Diseases (ISID)
-
European Society of Clinical Microbiology and Infectious Diseases (ESCMID)
-
Asian Pacific Society of Clinical Microbiology and Infection (APSCMI)
-
British Infection Association (BIA)
-
Australian Society for Infectious Diseases (ASID)
-
Japanese Association for Infectious Diseases (JAID)
-
Indian Association of Medical Microbiologists (IAMM)
-
Infection Control Africa Network (ICAN)
-
World Society for Virology (WSV)
Participants & Participation Options
-
Speaker: Deliver keynote or invited lectures, share research and innovations with global delegates.
-
Delegate: Attend sessions, panel discussions, networking events; access conference materials and expert interactions.
-
Poster Presenter: Showcase original research via printed or digital posters; engage in one-on-one discussions.
-
Exhibitor: Display products, technologies, or services; network with delegates and potential collaborators.
-
Video Presentation: Present research via recorded sessions; ideal for those unable to attend in person.
-
E-Poster Presenter: Share research electronically; participate in virtual Q&A and discussions.
-
Virtual Registration: Attend live-streamed sessions, access recordings, materials, and virtual networking; ideal for international participants.
Participant Benefits
-
Earn CPD/CME points
-
Networking with global experts and peers
-
Certificate of participation
-
DOI publication opportunities in conference proceedings
-
Access to cutting-edge research
-
Professional visibility for speakers, presenters, and exhibitors
-
Opportunities for global collaboration
Abstract Submission & Registration Timeline
-
Abstract Submission: Now Open
-
Early Bird Registration: April 20th, 2026
-
Standard Registration: June 10th, 2026
-
Final Registration Deadline: August 15th, 2026
Abstract Details: Peer-reviewed; accepted abstracts published in proceedings with DOI for global visibility. Authors receive an Abstract Acceptance Letter confirming inclusion.
Secure Your Place & Submit Your Abstract
Don’t miss the opportunity to participate, present your research, and network with global experts.
For Inquiries:























